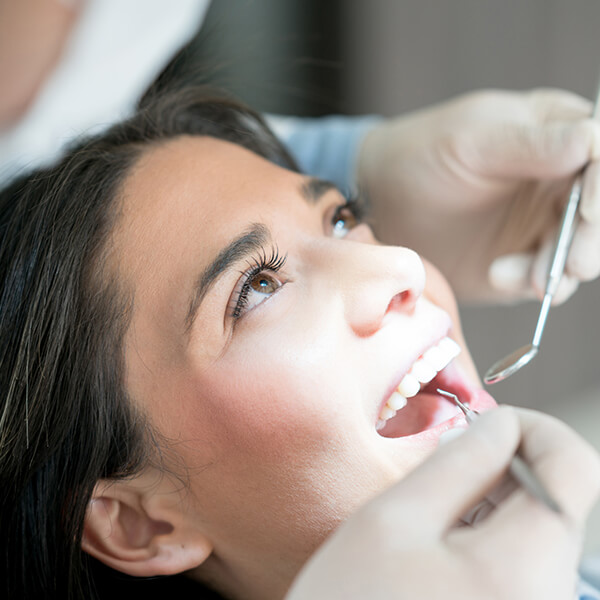
Periodontal Therapy
What Is Gum Disease?

In simple terms, look at your gums and bone around your teeth like the foundation of your house. Just like a house, the foundation must be sound regardless of the beauty of the home. When the foundation crumbles, the rest of it does too. This is what happens in gum disease.
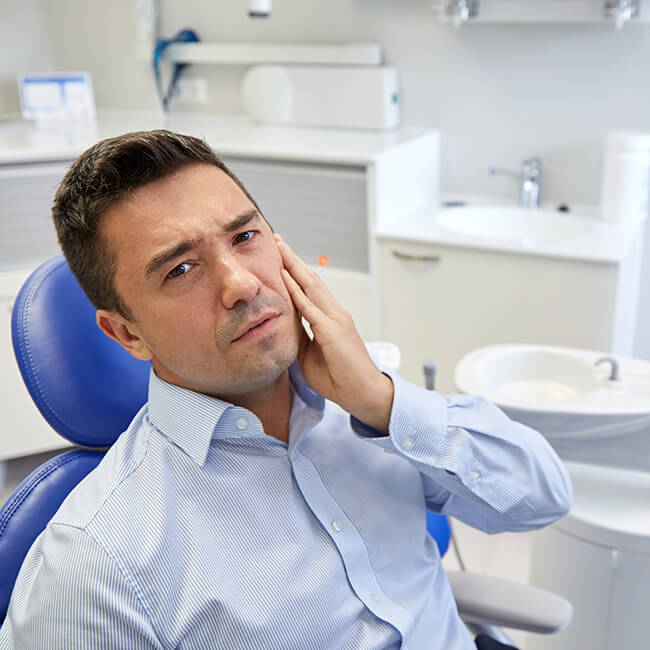
Gum disease, also known as periodontal disease, can advance with few signs or symptoms. Many patients diagnosed with this condition experience no pain and are surprised by the quiet yet swift damage that periodontal disease leaves in its wake.
While not curable, gum disease is controllable with regular professional hygiene appointments, dental exams, and consistent home care practices.
What Causes Gum Disease?

Our mouths provide a home to millions of bacteria, both beneficial and harmful.
Bacterial waste forms a sticky substance, called plaque, which adheres to our teeth and can mineralize into something called tartar. Tartar becomes a colony for more bacteria releasing toxins into the gums.
Around each tooth’s base, there is a collar of gum tissue that forms a small pocket. This warm, dark environment provides a perfect habitat for tartar and bacteria to infiltrate.
Your gums react to this bacterial invasion with an inflammatory response that results in bleeding gums, known as gingivitis. If untreated, this can create a chronic infection in your periodontal pocket, and, in many cases, your bone can begin to deteriorate around the teeth.
In advanced cases, untreated gum disease leads to abscesses and generalized tooth loss.

Periodontal Therapy: How It Works
Click on each image to learn more.
There are several factors we consider before we make a gum disease diagnosis.
The small collar of gum, or pocket, around each tooth is usually two to three millimeters deep. Dr. Caldwell or our hygiene team can measure and chart these areas using a small measuring device called a periodontal probe. If these measurements are more than three millimeters and bleed upon probing, then periodontal disease is present.
Dr. Caldwell will also evaluate your gums’ texture and shape and detect any movement in each tooth. It’s also vital to examine the bone’s levels, shape, and density around your teeth with digital x-rays. By collecting this data, a clear picture forms about your gum condition.
After establishing a diagnosis that defines your gum disease’s severity, we can develop a personalized treatment plan.
In milder forms with little or no bone loss, one or two visits with our hygiene team may bring the condition under control. You’ll leave our office with a daily home care strategy and an established professional maintenance schedule; little additional treatment may be needed.
If the inflammation has advanced and measurable bone loss is evident, well suggest a proactive approach to stop further deterioration. Over a few visits, we will gently numb your gums to perform root planning or scaling. The infected pocket around each tooth, including the mineralized tartar, must be carefully cleaned out with both hand and ultrasonic instruments. Polishing the teeth to create smooth surfaces that help repel stain and plaque accumulation usually finishes this initial therapy.
Dr. Caldwell may suggest a medicated rinse, an electric or ultrasonic toothbrush, and other specific strategies to help you with your home care routine.
Regular home care is critical to stop the progression of gum disease.
Within a few hours of cleaning, the bacteria begin to repopulate and adhere to the teeth. Plaque left undisturbed will start to harden and mineralize within 24 hours. Remember, deeper gum pockets require even more diligence to prevent the bacteria from undermining the foundation of your teeth.
Since gum pockets previously damaged by bacteria can be difficult to clean at home, a faithful maintenance schedule with us is essential. We can customize your plan to include two, three, or four visits a year depending on the severity of the disease, its response to treatment, and your home care consistency.
If our combined efforts don’t slow or stop your gum disease progression, we may refer you to a specialist known as a periodontist.
The relationship between a person’s oral health and their whole-body health has never been more understood than it is today. Studies show a link between oral bacteria and conditions such as heart disease, stroke, arthritis, Alzheimer’s, and even certain types of cancer.
Bleeding gums provide a direct pathway into the bloodstream, a journey that oral bacteria can quickly take. If an open wound existed on your skin, infection would be a concern. Gum tissue that bleeds should be looked at no differently.
Diabetes and other auto-immune disorders lower the body’s ability to fight infection, allowing uncontrolled gum disease to advance faster and with more destruction. Research also confirms that the inflammation in the mouth can aggravate diabetes, making it harder to control.
This two-way relationship between two chronic conditions emphasizes the importance of proper oral care.